CFTI Therapy Models
Ages 3-18
TF-CBT is a conjoint child and parent psychotherapy model for children who are experiencing significant emotional and behavioral difficulties related to traumatic life events. It is a components-based hybrid treatment model that incorporates trauma-sensitive interventions with cognitive behavioral, family, and humanistic principles.
Ages 0-5 Infant/Child Mental Health
CPP is a treatment for trauma-exposed children aged 0-5. Typically, the child is seen with his or her primary caregiver, and the dyad is the unit of treatment. CPP examines how the trauma and the caregivers’ relational history affect the caregiver-child relationship and the child’s developmental trajectory. A central goal is to support and strengthen the caregiver-child relationship as a vehicle for restoring and protecting the child’s mental health. Treatment also focuses on contextual factors that may affect the caregiver-child relationship (e.g., culture and socioeconomic and immigration related stressors). Targets of the intervention include caregivers’ and children’s maladaptive representations of themselves and each other and interactions and behaviors that interfere with the child’s mental health. Over the course of treatment, caregiver and child are guided to create a joint narrative of the psychological traumatic event and identify and address traumatic triggers that generate dysregulated behaviors and affect.
Ages 2-7
Parent-Child Interaction Therapy (PCIT) is a dyadic behavioral intervention for children (ages 2.0 – 7.0 years) and their parents or caregivers that focuses on decreasing externalizing child behavior problems (e.g., defiance, aggression), increasing child social skills and cooperation, and improving the parent-child attachment relationship. It teaches parents traditional play-therapy skills to use as social reinforcers of positive child behavior and traditional behavior management skills to decrease negative child behavior. Parents are taught and practice these skills with their child in a playroom while coached by a therapist. The coaching provides parents with immediate feedback on their use of the new parenting skills, which enables them to apply the skills correctly and master them rapidly. PCIT is time-unlimited; families remain in treatment until parents have demonstrated mastery of the treatment skills and rate their child’s behavior as within normal limits on a standardized measure of child behavior. Therefore treatment length varies but averages about 14 weeks, with hour-long weekly sessions.
Ages 5-17
Alternatives for Families: A Cognitive-Behavioral Therapy is designed for families who are referred for problems related to the management of anger and/or aggression, which include several behaviors on a continuum reflecting the use of coercion and/or physical force. Specifically, AF-CBT seeks to improve the relationships between children and their parents/caregivers who experience any of the following clinical concerns:
- Anger and verbal aggression, including emotional abuse
- Ongoing family conflict
- Child behavior problems, including physical aggression
- Threats or use of harsh/punitive/ineffective physical discipline or punishment
- Child physical abuse
Any and all of these patterns may be demonstrated by an individual caregiver or a child/adolescent, but they also may characterize the interactions of the family. Accordingly, AF-CBT targets individual caregiver and child characteristics, as well as the larger family context.
AF-CBT is a treatment based on principles derived from learning and behavioral theory, family systems, cognitive therapy, developmental victimology, and the psychology of aggression.
Cognitive Therapy (CT) has been rated by the CEBC in the area of Depression Treatment (Adult). CT is a form of psychotherapy proven in numerous clinical trials to be effective for a wide variety of disorders. The therapist and client work together as a team to identify and solve problems. Therapists help clients to overcome their difficulties by changing their thinking, behavior, and emotional responses. CT and Cognitive Behavioral Therapy are often used interchangeably. There are, however, numerous subsets of CBT that are narrower in scope than CT: e.g., problem-solving therapy, stress-inoculation therapy, motivational interviewing, dialectical behavior therapy, behavioral modification, exposure and response prevention, etc. Cognitive therapy uses techniques from all these subsets at times, within a cognitive framework. CT was developed by the Academy of Cognitive Therapy’s president, Aaron T. Beck, MD, in the early 1960s.
Art therapy is a distinctive type of mental health treatment that allows clients the chance to express their emotions in a way that other forms of therapy do not.
The art created by clients in therapy sessions can be used as a nonverbal method of telling a story from one’s life or revealing their emotions about an issue; in other cases, it can be used in conjunction with verbal descriptions of life events and feelings. Either way, art therapists may use sessions to gain knowledge about and interpret the content of clients’ inner lives. The process of creating art may allow clients to calm down from an intense emotional state, causing them to consider their situation more rationally; it may alternatively cause them to experience and describe emotions that they have previously found it difficult to articulate. Art therapy does not require its clients to be “good” at art, only open to the concept of using art as a nonverbal method of self-disclosure.
Art therapists are unique mental health therapists who receive specialized training in the practice of teaching clients to engage their minds and bodies in ways that are impossible with just verbal articulation. The legitimate practice of art therapy requires a master’s degree in the field, as well as licensure. They are knowledgeable in the study of art and psychology.
All ages (and some Adults too)
http://www.a4pt.org/page/ptmakesadifference
Through the play therapy process children create play that resembles the emotional experiences they are struggling with internally. These experiences usually cannot be expressed verbally. Children will select special toys to include in their play and use those toys to recreate issues that represent emotional conflicts that are important to the child. Beginning with this expression, the child’s play evolves until the child gains a sense of understanding and comfort over this situation. Research supports the effectiveness of play therapy with children experiencing: PTSD, behavioral issues, depression, impulsivity, self-esteem issues, academic difficulties, parent-child relationship struggles, social issues, anxiety, loss, divorce/separation, abuse and more… * Copyright 1998 Byron or Carol Norton
Animal Assisted Therapy
The formal definition of Animal Assisted Therapy: “AAT is a goal-directed intervention in which an animal that meets specific criteria is an integral part of the treatment process. AAT is directed and/or delivered by a health/human service professional with specialized expertise, and within the scope of practice of his/her profession.
AAT is designed to promote improvement in human physical, social, emotional, and/or cognitive functioning [cognitive functioning refers to thinking and intellectual skills]. AAT is provided in a variety of settings and may be group or individual in nature. This process is documented and evaluated.” (From Standards of Practice for Animal-Assisted Activities and Therapy)
AAT is used in counseling to assist with meeting the following goals:
- Improvement in Mental Health.
- Increase attention skills (i.e. paying attention, staying on task)
- Develop leisure/recreation skills.
- Increase self-esteem.
- Reduce anxiety.
- Reduce loneliness.
- Increase motivation.
- Improve willingness to be involved in a group activity.
- Improve interactions with others.
- Increase exercise.
Eye Movement Desensitization and Reprocessing (EMDR)
What is EMDR?
The mind can often heal itself naturally, in the same way as the body does. Much of this natural coping mechanism occurs during sleep, particularly during rapid eye movement (REM) sleep. Francine Shapiro developed Eye Movement Desensitization and Reprocessing (EMDR) in 1987, utilizing this natural process in order to successfully treat Post-traumatic Stress Disorder (PTSD). Since then, EMDR has been used to effectively treat a wide range of mental health problems.
What happens when you are traumatized?
Most of the time, your body routinely manages new information and experiences without you being aware of it. However, when something out of the ordinary occurs and you are traumatized by an overwhelming event (e.g. a car accident) or by being repeatedly subjected to distress (e.g. childhood neglect), your natural coping mechanism can become overloaded. This overloading can result in disturbing experiences remaining frozen in your brain or being “unprocessed”. Such unprocessed memories and feelings are stored in the limbic system of your brain in a “raw” and emotional form, rather than in a verbal “story” mode. This limbic system maintains traumatic memories in an isolated memory network that is associated with emotions and physical sensations, which are disconnected from the brain’s cortex where we use language to store memories. The limbic system’s traumatic memories can be continually triggered when you experience events similar to the difficult experiences you have been through. Often the memory itself is long forgotten, but the painful feelings such as anxiety, panic, anger or despair are continually triggered in the present. Your ability to live in the present and learn from new experiences can therefore become inhibited. EMDR helps create the connections between your brain’s memory networks, enabling your brain to process the traumatic memory in a very natural way.
What is an EMDR session like?
EMDR utilizes the natural healing ability of your body. After a thorough assessment and development of a treatment plan, you will be asked specific questions about a particular disturbing memory. Eye movements, similar to those during REM sleep, will be recreated simply by asking you to watch the therapist’s finger moving backwards and forwards across your visual field. Sometimes, a bar of moving lights or headphones or Tapping is used instead. The eye movements will last for a short while and then stop. You will then be asked to report back on the experiences you have had during each of these sets of eye movements. Experiences during a session may include changes in thoughts, images and feelings.
With repeated sets of eye movements, the memory tends to change in such a way that it loses its painful intensity and simply becomes a neutral memory of an event in the past. Other associated memories may also heal at the same time. This linking of related memories can lead to a dramatic and rapid improvement in many aspects of your life.
What can EMDR be used for?
In addition to its use for the treatment of Post-Traumatic Stress Disorder, EMDR has been successfully used to treat:
anxiety and panic attacks depression, PTSD anger phobias
sleep problems
grief and loss addictions pain, including phantom limb pain performance anxiety feelings of worthlessness/low self-esteem
Before and after EMDR brain scans.
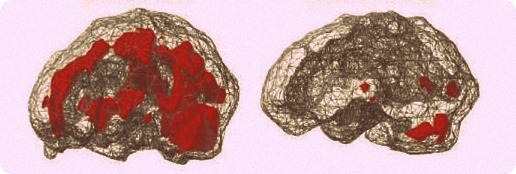
Left photo shows woman with Post Traumatic Stress Disorder. Right photo shows same woman after four ninety minute EMDR sessions. The brightened areas indicate over-activity in the brain. Photo by Dr. Daniel Amen
Can anyone benefit from EMDR?
EMDR can accelerate therapy by resolving the impact of your past traumas and allowing you to live more fully in the present. It is not, however, appropriate for everyone. The process is rapid, and any disturbing experiences, if they occur at all, last for a comparatively short period of time. Nevertheless, you need to be aware of, and willing to experience, the strong feelings and disturbing thoughts that sometimes occur during sessions.
How long does treatment take?
EMDR can be brief focused treatment or part of a longer psychotherapy treatment plan. EMDR can be easily integrated with other approaches in which your therapist might be trained, such as Psychodynamic psychotherapy, Dialectical Behavior Therapy, or Cognitive Behavior Therapy. For best effects, EMDR sessions during the actual reprocessing phases of treatment usually last from 60 to 90 minutes. Positive effects have been seen after one session of EMDR.
Will I will remain in control and empowered?
During EMDR treatment, you will remain in control, fully alert and wide-awake. This is not a form of hypnosis and you can stop the process at any time. Throughout the session, the therapist will support and facilitate your own self-healing and intervene as little as possible. Reprocessing is usually experienced as something that happens spontaneously, and new connections and insights are felt to arise quite naturally from within. As a result, most people experience EMDR as being a natural and very empowering therapy.
What evidence is there that EMDR is a successful treatment?
EMDR is an innovative clinical treatment that has successfully helped over a million individuals. The validity and reliability of EMDR has been established by rigorous research. There are now over nineteen controlled studies into EMDR, making it the most thoroughly researched method used in the treatment of trauma, and The American Psychiatric Association, American Psychological Association, Department of Defense, Veteran’s Administration, insurance companies, and the International Society for Traumatic Stress Studies recognize EMDR as an effective treatment for PTSD. For further information about EMDR, point your Internet browser to www.emdria.org or www.emdr.com.
